Researchers from the University of Michigan Rogel Cancer Center and School of Dentistry, led by Dr. Yu Leo Lei, have made an important discovery regarding the impact of obesity on oral cancer and its ability to evade the immune system. Their findings, published in Cell Reports, shed light on how obesity creates a tumor microenvironment that supports the progression of oral cancer. The study reveals the intricate relationship between saturated fatty acids, the STING-type-I interferon pathway, and NLRC3.
Traditionally, obesity has been associated with an increased risk of gastrointestinal tumors, breast cancer, pancreatic cancer, and ovarian cancer. However, recent large-scale studies involving millions of individuals from various regions have uncovered a previously underestimated connection between obesity and oral cancer risks. Dr. Lei, a pathologist-immunologist and the lead author of the study, explains that this research establishes the first mechanistic link between obesity and immune evasion in oral cancer.
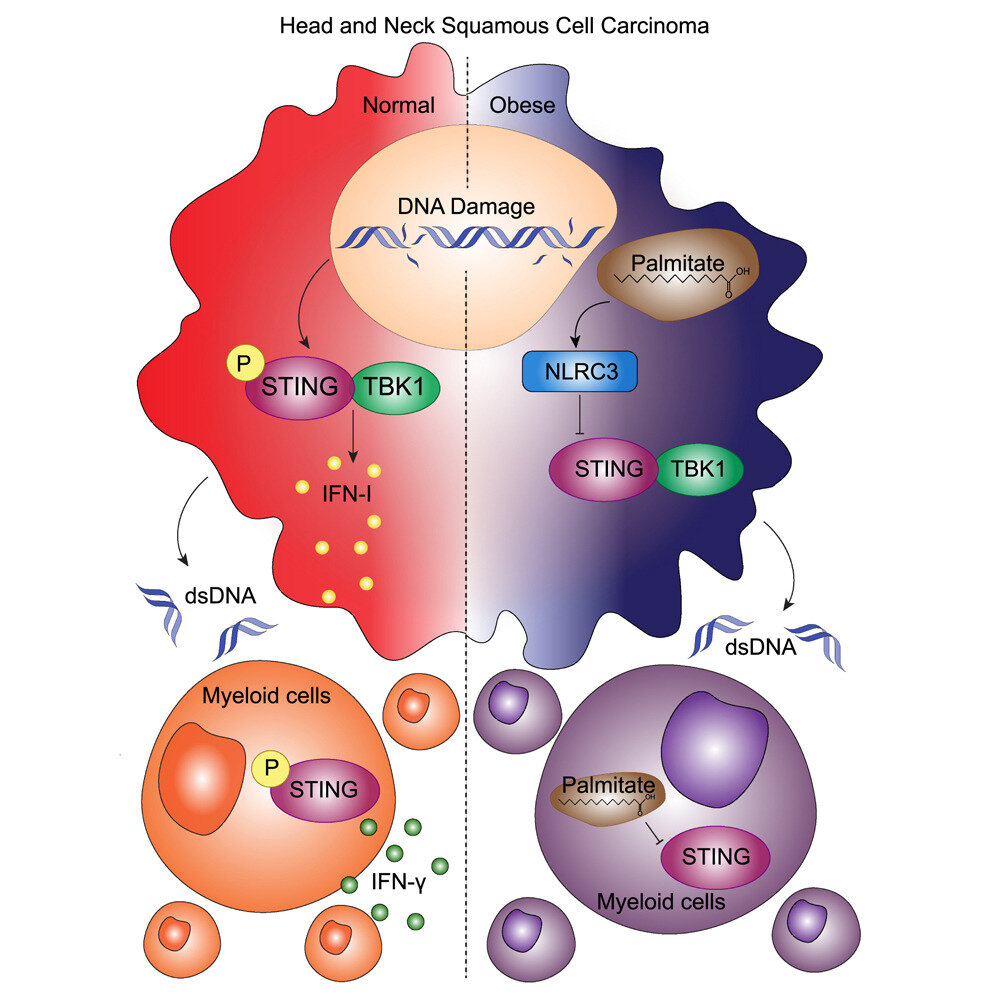
The team observed that myeloid cells in obese mice demonstrated insensitivity to STING agonists and exhibited greater suppression of T cell activation compared to myeloid cells in lean hosts. This characteristic contributed to the depletion of immune subsets essential for anti-tumor immunity in the tumor microenvironment.
The researchers discovered that saturated fatty acids hinder the STING pathway, which is responsible for inducing the maturation of antigen-presenting cells in response to cytosolic DNA. This obstruction is caused by the production of a protein called NLRC3.
Dr. Lei highlights the potential translational implications of these findings and mentions two recent studies that demonstrated improved overall and cancer-specific survival in oral cancer patients who were prescribed statins, cholesterol-lowering medications. According to him, this study establishes a mechanistic connection between those observations and emphasizes the possibility of targeting fatty acid metabolism to modulate the host’s anti-tumor immune response.
Moving forward, Dr. Lei’s team intends to investigate how obesity influences other immune-activating pathways and identify novel targets for interventions aimed at better oral cancer prevention in high-risk individuals. However, further research is necessary before these findings can be translated into clinical applications.
Additional authors of the study include Dr. Blake Heath, Dr. Wang Gong from the School of Dentistry, and Hülya Taner, a D.D.S.-Ph.D. candidate.
Source: University of Michigan